By: Tom Davis, VP of Clinical Operations-Physical Therapy
In our prior blogs, we’ve discussed some of the roadblocks that get in the way of our vision of a PT First approach to musculoskeletal (MSK) care like high patient payment responsibility or administrative hassles. But even if we managed to remove those obstacles, our vision for PT First can only become a reality if we provide the best possible patient experience with the best possible outcomes. To do so, we’re working to integrate the most-up-to date clinical guidelines for MSK conditions into our standard of care. We’ll discuss these efforts in our next blog. However, even if we succeed at implementing the best standard of care, there’s only so much we as providers can do to ensure clinical success. In physical therapy, perhaps more than in any other clinical field, success depends on enlisting patients in their own care. They are the ones who have to show up to their appointments, they are the ones who have to follow up with at-home exercises, they are the ones who have to adopt healthier lifestyles. If we’re not able to encourage them to do this, then they fail and we fail.
So how do we engage patients? Driving patient compliance, after all, is notoriously difficult to accomplish. We Americans don’t want to be told what to do, even if it’s good for us. There’s a reason why Americans’ health is declining, obesity is rising, and chronic illness continues to increase throughout the United States. Over the years, though, we at Cypress Health Partners have discovered some tried and true ways to enlist patients in their own care, effectively reducing MSK injuries and improving patients’ overall wellness.
It starts when patients first enter our clinics. For patients to be compliant and to stay on their care plan, it’s essential that we as providers understand what brought them to us in the first place. The answer can’t just be, “I have pain and weakness in my shoulder.” That’s usually not the issue. So we need to keep asking, “What really brings you here?” And eventually, they’ll say, “I can’t put my coat on without help”, or “I can’t pick up my grandson,” or “I can’t enter my sorority pickleball tournament because I’m in wincing pain when I hit an overhead.” Now we’re getting to the personal reason why they’re at the clinic. From there we develop a care plan, with clear milestones for reaching their goal which is a lot less about their actual impairment than about the part of their life they want to fix—like picking up a grandson.
When a patient is emotionally invested in the outcome of their plan, they’re much more likely to be engaged in their own success. But even though we might successfully engage our patients, some might not be fully committed to what we know is needed for success. That’s why education at the beginning of treatment is essential. For some conditions, for instance, it’s optimal for patients to come to the clinic three times per week instead of two times per week. We developed a chart for patients who are concerned that coming in three times per week is too time-consuming or too expensive. The chart shows that patients who come in three times per week recover almost three weeks faster than patients who come in only twice per week.
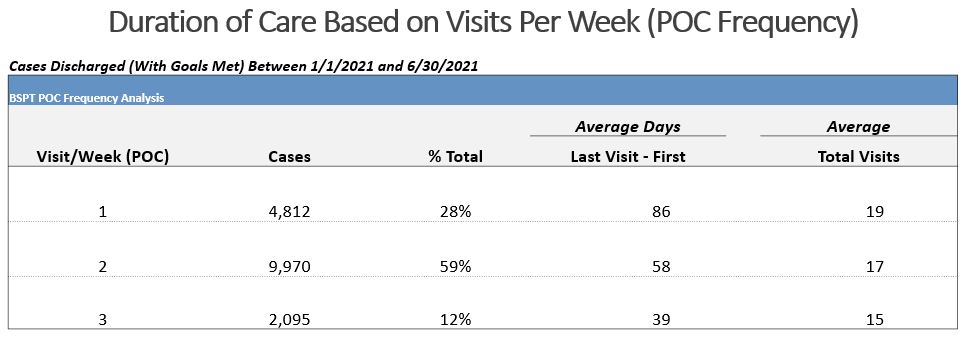
Patients and the medical community need to buy into this care plan in order for it to be successful. It’s hard to argue with this type of evidence gathered from over 15,000 new patients seen. Through this data, we’ve learned that the prescribed frequency of care and early access to care in the beginning, is shown to reduce cost, improve outcomes and improve patient experience.
Some patients might also worry that they can’t cover so many co-pays in such a short period of time. In that case, we’ll work with them to create a payment plan they are comfortable with. This helps reinforce that we are invested in their success, which can only be achieved if they invest the time required upfront.
Once patients’ care begins, we help ensure they adhere to their plan of care by regularly showing them their progress. During most visits, I show patients how their range of motion, strength, or balance has improved — and make the connection between the intermediate work they’re doing and their improvement against their goal. Seeing improvement motivates the patients to stay actively engaged in their recovery. Or sometimes when we look at a patient’s progress, we’ll see that the patient is not progressing against their plan. In many cases, this will reveal that patients are not doing all their exercises, which is a good opportunity to remind them that they won’t achieve their personal goals unless they put in the required effort. When patients see how they might not progress toward a goal they’ve set for themselves, like picking up a grandchild, they’re much more accountable to themselves and to us. The next time they visit, they’re motivated to show us —and themselves— that they’re progressing. Sometimes, however, a lack of progress indicates that we need to alter a plan of care. This is a good opportunity to show the patient that we’re on the same team, continually evaluating and re-assessing the care plan toward the ultimate success of the patient.
At Cypress Health Partners, success in meeting a patient’s goal is usually the beginning of a patient engaging in their care with us, not the end. Success helps us build a trusting relationship with the patient which is essential for compliance. When the patient leaves the office able to swing her pickleball paddle overhead without wincing in pain, I remind her that she’s responsible for her wellness over her lifetime. I tell her that if she has the slightest bit of discomfort in her shoulder—or perhaps new soreness in her hip or knee— she should contact us immediately so that we can address the problem together before it becomes so painful that she can’t do what she enjoys. These opportunities help us underscore the importance of patients partnering with us in preventative care – or what we call well care versus sick care — which is ultimately the most cost-effective and least invasive way for our patients to stay healthy and fulfilled.
We’ll cover the topic of well care vs. sick care in more depth in one of our upcoming blogs.
Please share your thoughts in the comments below.
